
In the spring and early summer of 2008, Pete O'Donovan underwent two surgical operations to his hands to alleviate a disabling condition known as Dupuytren's Contracture. Despite medical opinion to the contrary, Pete thinks his problems were almost certainly a direct result of climbing.
This article was first published on UKC in 2008 and has been reformatted in 2010 to fit with our redesigned site.
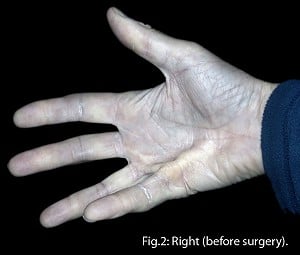
Dupuytren's Contracture and Climbing
As one of an ever-increasing number of committed long-term climbers (i.e. 20+ years experience), I suspect I am far from alone in a growing realization that, while climbing may generally be regarded as having beneficial effects on ones health, pushing things to, and beyond ones personal limits on a regular basis will eventually leave a legacy of injuries and ailments, a permanent reminder of past conquests (and failures!) to take into old age.
My personal 'Butcher's bill' is probably fairly typical through the years: sprained and broken bones, pulled muscles and tendons, torn ligaments, etc. Most have healed reasonably well, though the metal screws and plates in my left heel and wrist still make their presence felt every time the weather takes a turn for the worse. I'm not complaining; for a bloke of my age, thirty-odd years high- level involvement in just about any sport would have probably yielded similar results. In fact, judging by the numbers of 'silver crimpers' I see on the crags and walls these days, it may well prove that climbing is one of the gentler activities for the ageing sportsman. That said, in terms of anatomical abuse, there is one area of a climber's body, which, in comparison with other sports, is particularly at risk — the hands. OK, they were designed for climbing — one only has to think of our near evolutionary neighbours swinging effortlessly through the jungle to realize this. However, trees are one thing; steep rock is quite another. Take Granite, for example; cramming one's digits into thin, vertical cracks, then twisting the hand to achieve the necessary 'torque' is surely a very long way from what nature intended. I can still remember during my 'Yosemite' years, the knuckles becoming so swollen by the end of the season I could hardly make a fist, and thinking: "hmm, this can't be that good for you". Or what about limestone, with it's tiny, sharp edges and dynamic moves on one and two-finger pockets? Hardly a recipe for happy hands in the long run.
And so, when during the early '90s, I started to get hard, painful, little lumps in my palms, which later developed into cords and began deforming the fingers, it seemed entirely reasonable that, whatever was going on, climbing abuse was almost certainly responsible. It came as some considerable surprise then, to find that my 'Dupuytren's Contractions' (as it was later identified) is a relatively common condition and one to which very few hand specialists attribute any connection at all with rock climbing, or indeed any other form of physical activity. However, for something that affects so many people worldwide, research into Dupuytren's has thus far been both minimal and inconclusive. Maybe this is not so surprising? After all, it's non-fatal, slow to progress, largely painless and affects mainly older people, so who cares? Well, perhaps young rock climbers should, because despite what many experts in the medical profession might say, there's increasing evidence to suggest that high-level participation in our particular sport gives rise not only to a much greater incidence of the condition than in the general population, but also its onset at a far earlier age. Read on.
What is Dupuytren's Contracture?
In simple terms Dupuytren's is a disease affecting the connective tissue of the palms (known as the palmar fascia), which lies between the skin and underlying muscles and tendons. The name derives from a 19th century French anatomist and military surgeon, Baron Gillaume Dupytren, who is credited with carrying out the first successful operation to alleviate the condition. The initial signs are the aforementioned lumps, or nodules, most commonly appearing near the base of the fingers, but sometimes occurring throughout the palm, or more rarely, in the digits themselves. The lumps may be quite tender — I seem to remember some discomfort at the time, though this was possibly due to the over-enthusiastic efforts of my physiotherapist to 'massage them away' (at £60 an hour!) which ultimately proved fruitless. This stage of the disease may also be characterized by pitting and puckering of the skin surface. The next phase is the development of cords, generally following the lines of the tendons, which, over a period of time (and here we are probably talking several years) develop and thicken, then begin to contract, pulling the fingers in towards the palm. The little and ring fingers are most commonly affected first, and in extreme cases the hand becomes so deformed that the fingernails actually dig into the skin of the palm, though most patients would hopefully seek medical intervention long before this happens. The cords are formed by deposits of Collagen, a protein occurring throughout our bodies in various forms and the main ingredient of scar tissue. But exactly what causes it to behave in this 'rogue' fashion is still a matter of some debate.
The Causes of Dupuytren's
Most experts seem to agree that the typical Dupuytren's patient would be: a) male, (women make up only about 20% of sufferers); b) aged at least 50; c) of northern European (Viking) descent and d)with a family history of the condition. At the time I began developing the Dupuytren's, I only really qualified in the first of those categories (male). The Nordic link does, however, seem valid, as the first person I ever met with Dupytren's was a guy called Rory Gregory — a brick s***house of a bloke with long, straw blond hair and piercing blue eyes — the epitome of the Viking warrior as portrayed in the modern media. Have you ever seen the 1959 classic Hollywood romp The Vikings? Well, Rory so looked the part that he made Kirk Douglas' lead character, Einar Ragnarsson, appear positively effeminate. If Rory had played the role, there's absolutely no way the wimpy half-brother (Tony Curtis) would have managed to duck in under Einar's sword arm and deliver that fatal thrust in the final scene, with or without those ridiculously short shorts! But I digress. Beyond these basic indications, the causes of Dupuytren's become far from clear, but among the most popular 'secondary' links currently in vogue are: Diabetes, alcohol and tobacco abuse, drugs used to control Epilepsy and sudden trauma, i.e. serious injury to the hand or forearm. Involvement in manual work or certain sports comes well down the list, but this is one area of interest I believe merits far closer scrutiny.
Dupuytren's and Climbing
This is not the first time a link between high-level rock climbing and Dupytren's has been suggested. In 2005 the British Journal of Sports Medicine published the results of a questionnaire-based study carried out amongst members of the Climbers Club, asking individuals to report on potential symptoms of the condition, as well as any possible contributory factors, such as age, alcohol consumption, etc. Whilst not exactly scientific, the report concluded that climbers were several times more likely to develop Dupuytren's than members of the general public. Furthermore, those with the disease revealed a significantly higher lifetime intensity of climbing activity (in both frequency and level) than those without. This study was originally brought to my attention by one of the members of this very forum, who in his post jokingly observed that "Beard ownership, beer drinking and wearing a Whillans harness were obviously high risk factors" The average age of Climbers Club members is probably quite high (50's?), but evidence of Dupuytren's appearing in a much younger generation can be found in the pages of the UK Bouldering forum: http://ukbouldering.com/board/index.php/topic,4609.10.html .
So how exactly might climbing be the catalyst for Dupuytren's? One recent theory, though not actually related to climbing as such, suggests that micro-trauma — repeated minimal damage, causing chronic inflammation of the tissue could be to blame. This may occur as a result of, say, slapping for large, rounded holds. Personally, I've never really been one for dynamic moves, preferring control where possible, but if memory serves correct, around the time I first noticed the nodules I'd been doing a lot of training on a little wall I had set up in my workshop, on which 'power-endurance' circuits would invariably finish with a desperate lunge for one of the larger holds at the top. Of course, for the hard-core boulderer, 'slapping one on' is part and parcel of the game. Perhaps the body tries to repair these repeated micro-traumas and, over time, lays down excessive amounts of scar tissue, thus kicking off the whole Dupuytren's process?
Treatment
Dupuytren's can be so slow to progress and its effects so varied that many will choose simply to live with the condition. For others, like me, the ensuing deformities eventually warrant some kind of medical attention. Here are the choices.
Surgery
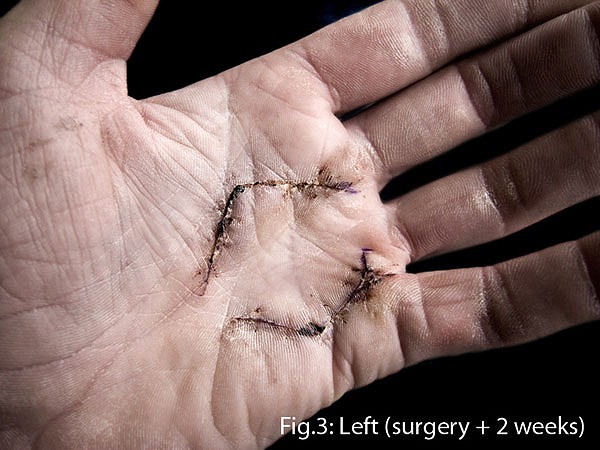
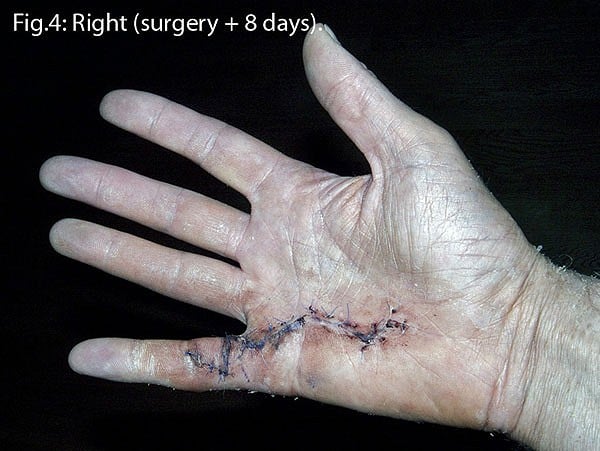
When the disease has progressed to the stage where one or more fingers is bent in towards the palm at an angle greater than 20°, surgery is the solution most hand specialists currently suggest. The operation, known as a fasciectomy, is normally conducted under a local anaesthetic nerve block and aims to completely remove the affected tissue (cords). Zig-zag incisions are used (Figs.3&4) as opposed to straight cuts, as this reduces the affects of shrinkage as scar tissue forms during the healing process. Following surgery a splint is worn for up to six weeks, initially 24 hours a day, then just while sleeping. Once the stitches are removed (after 2 weeks) it is of paramount importance that the patient continually stretches and massages the hand in order both to increase mobility and reduce the build up of scar tissue (Figs.3-7).
A successful outcome i.e. returning the hand to maximum function, where the fingers can be fully extended, depends on several factors: the age of the patient, the level of deformity before surgery and the original location of the cords. Where cords extend right up to the middle (PIP) joint of the finger, the prognosis for complete recovery is lower than for entirely palm-based cords. Likewise, the likelihood of re-occurrence (a problem with all Dupuytren's treatments) is greater in this instance. Surgery always carries risks, not the least of which is an outside chance of nerve damage, either temporary or permanent, though the latter is apparently very rare. But for the keen climber, perhaps the major drawback of surgery is the length time needed for full recovery — at least 6 weeks (per hand) in most cases.
Needle Aponeurotomy
Needle Aponeurotomy, also known as NA, was originally pioneered in France around 20 years ago, but is now gaining increasing acceptance around the world. The procedure involves inserting needles directly into the cord at various points, thus weakening it until it can actually be mechanically broken and the tension relieved. The main advantage of NA is that it is a minimally invasive technique, conducted under local anaesthetic, and has a very short recovery period (2-3 days). The main disadvantage is that re-occurrence rates are extremely high — the cord invariably re-forms, though sufferers may experience several years of 'normal' use and the procedure can be repeated several times. Proponents of this form of treatment suggest it as a sensible first port of call, which, at best, may produce excellent results and, at worst, delay the need for surgery by several years. After all, surgery is still possible after several NA treatments, but not visa-versa. Although it is possible to receive NA treatment on the NHS, it seems likely that few GP's will have actually heard of it yet, let alone have an informed opinion!
Xiaflex™
Xiaflex™ is the name of a new drug being developed by Auxilium Pharmaceuticals, which is currently undergoing clinical trials in the United States and Australia. The treatment is not dissimilar to NA, with the addition that the drug (based on Clostridial Collagenase) is injected into the cords with the aim of lysing (breaking apart the cells of) the tissue over a period of time. It sounds very interesting, but only time will prove its effectiveness.
Radiotherapy
This is a relatively recent addition to the arsenal of weapons deployed against Dupuytren's, and currently the only treatment designed to tackle the disease at an early stage. In very simple terms, low-level rays are delivered to the affected area (nodules) over several sessions. Apparently, early indications are very favourable. Radiotherapy actually seems capable of stopping the growth of nodules or cords either permanently or for a reasonable length of time; sometimes nodules disappear completely. However, radiotherapy cannot make an already bent hand straight again. Unfortunately this treatment is available in very few clinics, possibly none at all in the UK, although Poole Hospital is listed as one possible location on one of the websites I've listed below.
A Summary
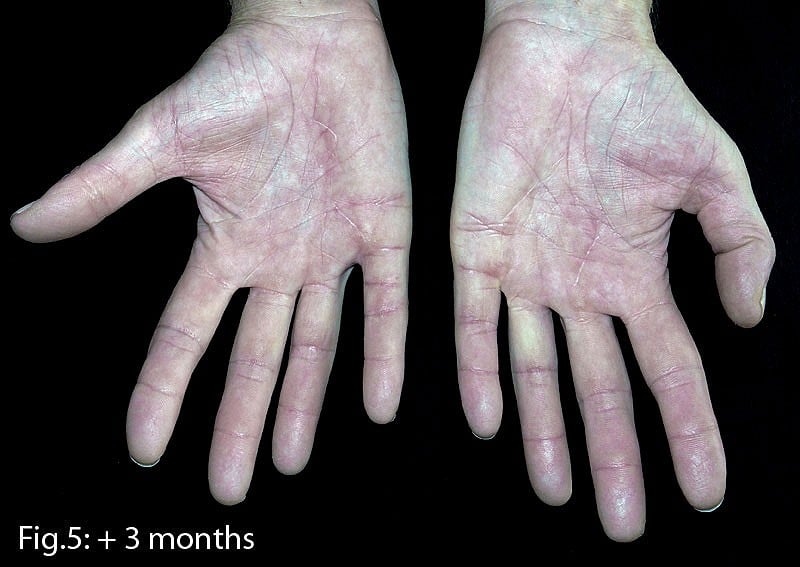
As someone who's currently in the process of trying to claw my way back to fitness, after being off the rock for nearly four months, I now feel that if I'd had all this information at my disposal a few years ago I might have done things rather differently. Don't get me wrong — the results from my surgery are excellent (Fig.5) and the team at Sheffield's Northern General Hospital first class. I'm sure I'd have ended up needing surgery at some stage of my life, but if I had my time again, I think I would almost certainly at least try NA first. Just out of morbid curiosity, I recently emailed the 'before' pictures of my hands to Chris Bainbridge (who later proved a very valuable source of information while preparing this article) at the Bainbridge Hand Clinic in Derby, one of the foremost practitioners of NA in the country. I read his reply with mixed emotions, the gist of it being that my Dupes would have been the perfect 'candidates' for this particular treatment! Oh well, we live and learn.
For the future, it seems likely that more and more time and funds will be devoted to seeking non-invasive treatments for Dupuytren's. The initial indications of the Xiaflex™ trials are encouraging, as is the reported success of radiotherapy in tackling the disease at an early stage. Unfortunately the costs involved in both these treatments may be prohibitive for our poor, old, cash-strapped NHS, though traditional surgery, requiring a team of at least six medical staff (including surgeons and anaesthetists) and an hour in theatre, must surely prove a bigger drain on resources in the long run
A wealth of information about Dupuytren's appears on the web; here are a few of the more useful sources:
Please note: I am in no way medically trained or qualified and the above article is purely a reflection of my personal research and experience.

About Pete O'Donovan:
Pete O'Donovan (49) of Sheffield and Spain, started POD in 1983 making rucksacks, chalkbags and more recently bouldering mats. He is a talented climber and photojournalist. You may have seen his poster prints in some climbing shops and several climbing magazines like Desnival and the USA's Urban Climber magazine. You can see some of his excellent work at his UKClimbing.com photo gallery here: GALLERY
Last year he sold POD to Equip Outdoor Technologies although he is still involved with POD as designer, consultant, adviser and overseer of quality control. Pete and his wife, Angels, can now spend more time climbing after many years huddled over sewing machines.
We wish Pete a fast and complete recovery from his operation and would like to thank him for sharing his experiences with UKC












Comments